For many years, operation rooms have faced more than one predicament. Recently, in obstetrics, nurse and nurse’s aide did over 700 ghost surgeries. Many countries are concerned about the problems that could happen in the operation rooms; they take the form with ghost surgery, sexual harassment and professional negligence. For example, the United States of America(USA) also tried to make a regulation about the operation room CCTV in 2015 but it didn’t pass the National Assembly, so it just ended as try. So, the regulations and laws are erected but none of them could prove effective against them. Recently, Gyeonggi province decided to install CCTV in the operating room. The argument as to the feasibility of this measure has been undergoing vigorously in society.
 |
| ▲ Surveillance system have been urged to be set up in operation room to protect the patients' rights (Photo by 123rf stock photo) |
It’s true that privacy within the operating rooms is needed for hygiene and patients’ safe so from now on, every surgical process is unopened to us. Otherwise, it can also cause some side-effects, so many patients argued to be transparent. Nobody knows what is actually going on in the operating room except medical staff. There are some people in the medical field who exploit this right and leave their ethics behind. One of the most severe problems is known as ‘ghost surgery’. Ghost surgery refers to a situation of changing a patient’s surgeon without prior agreement. When a medical accident occurs due to a ghotricsst surgery, the patient's life is threatened.
Respect for the privacy of operating rooms means that the doctor is not available in the event of a change or any accident. An assistant-nurse in a hospital in Ulsan is accused of ghost surgery. He was involved in 17% of the overall surgery operated in the hospital. It turned out that he operated cesarean and urinary incontinence surgery over 700 times starting from December 2014. That hospital’s surgeon allowed the nurse to do surgery while he treated other patients. Similar cases happened in a Busan orthopedic hospital, too. Even the ghost surgery led to a surgical failure. The director of the hospital ordered a salesman from the hospital’s medical equipment supplier to operate on a patient’s shoulder instead of performing it himself. In this surgery, the patient had a cardiac arrest and fell into brain death.
Sexual harassment is another problem in the operating room. March, 25th, 2013, a woman felt the sudden fear of having a cosmetic surgery and she took voice recorder with her. After the surgery, she heard some sexual comments going on throughout her operation from the recorder. Some sayings like “Do you think she shaved?”, “I don’t think she has a boyfriend.” Women are not only victims of sexual harassment during the surgery. A male patient who had a double-jaw surgery also suffered from sexual harassment. The recorded conversation includes personal insults like “I think he is getting ready for transgender.” “He is not ugly but not likable either.” Patients under anesthesia are unable to know any of these incidents in the operating room.
There are several reasons as to why these problems keep repeating and the biggest reason is that the hospital can save money. If a doctor doesn’t do the surgery by himself and leave his operating authority to other nurses, then the hospital can reduce the costs because it can handle more surgeries. Also, interests between medical staff such as doctors and nurse and hospital’s manager, fit each other. If a doctor turns over his duty to other, then he can manage more patients so that his income inclines. And for the staff, he can sell his medical devices to the hospital so that his sales would go up.
Because of these reasons, lots of hospitals are doing the so-called ‘ghost surgery’, the operation managed by other doctors unknown to patients, and make more money. The law says a person who does the ghost surgery and person who made him or her to do the surgery, together with the doctor, would both face punishments.
First, according to the medical law, ghost operator may be subject to up to 5 years in prison or a fine of up to 50 million won, since he did medical practice even he is not the appropriate medical personnel. Second, according to the Act on special measures for the Control of health offenses, if the ghost operator keeps operating without a medical license, he or she can be subject to more than two years or be sentenced to life. Additionally, the hospital who made the ghost surgery can be subject to a business suspension or business cancellation within a period of one year.
As this practice has continued to raise the attention of many people, including both the hospitals and the patients, many have proposed the implementation of a surveillance system within the operating rooms. However, the process to make it possible has proved to be more difficult than it seems as they are people who agree and people who are against it.
Recently, Gyeonggi Provincial Medical Center, an organization governed by Gyeonggi Provincial Government to supervise all the hospitals in the province and foster cooperative activities in accordance to the fair medical practice, has decided to install CCTVs in the hospitals with the medical personnel’s consent. The chairperson, Lee Dong-wok claimed that as the decision concerns the privacy of both surgeons and patients, as well as the trust towards ‘the people who have sworn to serve the community of Gyeonggi province’, the hospital will only set up CCTV inside operation room with an agreement between the doctor and the patient.
Concerning the issue, the Dankook Herald conducted an interview with Kim Yong, a spokesperson from Gyeonggi Provincial Government about the current situation of pushing the surveillance system in all hospital across Gyeonggi Province. According to Kim, the system has been currently tested out Anseong Hospital in priority, the provincial government plans to expand it to other public medial institutes by early 2019. For now, Anseong Hospital are operated in ways of the patients can choose whether to have their operations recorded or not, and the file will be kept for a month before it is finally being discarded.
 |
| ▲ Photo from the interview with Kim Yong, the spokesman of Gyeonggi-do Province. |
The main opinion of those who opposite CCTV, which is impossible to respect for the privacy of patients, Kim stated that in order to secure the patients’ confidentiality and prevent leakage, they have been setting up guidelines for the management and protection of the patients’ video. Kim said that Anseong Hospital, which is currently running a CCTV trial operation, prepared the requirements for operation of surgical video processing equipment and policies for operation and management, also the consent of the information driven operating room staff was also obtained. That includes how the captured video clip of the operation would be stored, to the eventual disposal of the file. Within 30 days, the patient could request for verification of the operation process by viewing the video file.
As to how the people have responded to such implementation, Kim shared that about 91% of the residents in Gyeonggi province agreed to the new policy while 87% of them would agree to record their operation process in CCTV. Although it is not long since it was introduced and it is currently being operated only at Anseong Hospital, it is planning to expand its operation to six medical centers by 2019. Furthermore, in the future, they’ll try to expand the policy to private hospitals as well as public hospitals.
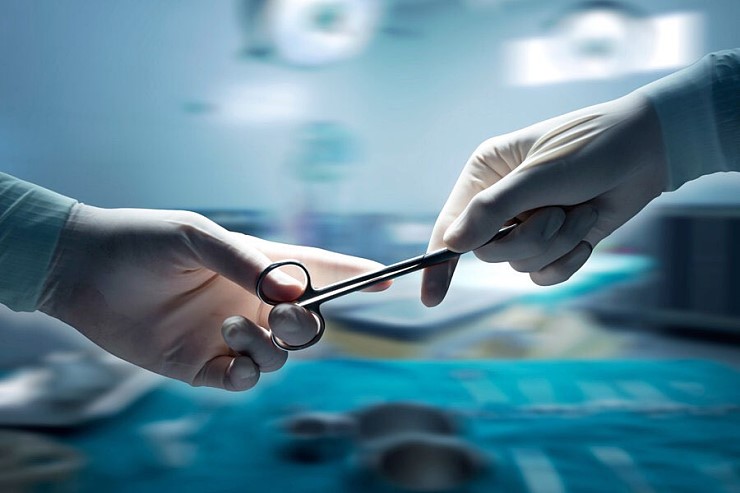 |
| ▲ In order to prevent ghost surgery, CCTVs are under discussion. (photo by Pulse) |
It is fair to say that new problems can be caused by applying CCTVs in the operating rooms but it is also true that the existing problems can be diminished. As the interviewee, Kim insisted, patients are the most vulnerable entities during the operation. If there is a problem, the patients’ rights have to be protected. The CCTV monitoring system in the operation rooms is one of the ways. Introducing CCTVs can be seen as a systemic and institutional aspect, and the underlying system to prevent such accidents from happening is to strengthen medical staff educations. Kim hopes the medical community will consider that CCTV serves as a net function to dispel public distrust and protect the majority of good healthcare workers due to a small number of insensitive caregivers.
Edward Ng, 김동은, 신지희, 한혜원 dankookherald@gmail.com
![[Campus Magnifier] Let's Surf the Library!](/news/photo/202404/12496_1765_4143.jpg) [Campus Magnifier] Let's Surf the Library!
[Campus Magnifier] Let's Surf the Library!
![[Campus Magnifier] Let's Surf the Library!](/news/thumbnail/202404/12496_1765_4143_v150.jpg)





